With our vision of patient-driven care for all Canadians, along with ground-breaking CANet-funded research, we continue to assemble innovative digital health technologies.
Apart from VIRTUES, our patient-centred digital health care platform, several of our successful research programs have a global impact.
(2015 – 2023)

John Sapp, CANet Investigator
Results published in the New England Journal of Medicine showed that catheter ablation more effectively reduced the incidence of recurrent arrhythmias and death than drug therapy.
Hospital News
An international study conducted by the VANISH2 Study Team has demonstrated the superiority of catheter ablation over antiarrhythmic drug therapy for patients with ventricular tachycardia, a potentially life-threatening heart rhythm disorder. The study compared the standard treatment for suppressing these dangerous rhythms with antiarrhythmic drugs against catheter ablation. This minimally invasive procedure targets and neutralizes abnormal heart tissue, causing short circuits in the heart’s electric system. This research represents a significant advancement in arrhythmia management.
Results published in the New England Journal of Medicine showed that catheter ablation more effectively reduced the incidence of recurrent arrhythmias and death than drug therapy. Furthermore, patients undergoing ablation did not have an increase in severe side effects, highlighting its potential to improve the quality of life for those battling ventricular tachycardia.
Focusing on safety and efficacy, the VANISH2 team noted that ablation provides long-term benefits by directly addressing the underlying electrical disturbances in the heart. These findings suggest a paradigm shift in treatment approaches, positioning catheter ablation as a preferred first-line therapy for many patients.
“Our findings demonstrate that catheter ablation should be considered a reasonable first-line treatment for ventricular tachycardia,” says John Sapp, CANet Investigator and principal lead of VANISH2. “By directly addressing the heart’s electrical dysfunction, we can significantly reduce arrhythmias and shocks from defibrillators, offering patients a better quality of life.”
▼ show more
Beyond individual patient outcomes, the study’s findings have significant implications for healthcare systems. Ventricular tachycardia is associated with high hospitalization rates and considerable healthcare costs. Early interventions like catheter ablation could significantly reduce these burdens, offering substantial savings and improving overall system efficiency, providing a strong motivation for healthcare policymakers to adopt these findings.
As arrhythmia-related hospitalizations continue to rise globally, the study sets a precedent for adopting evidence-based, cost-effective treatments.
▲ show less

Stephen B. Wilton, CANet Investigator
CANet-funded study found that one in three patients with reduced cardiac muscle function after a heart attack did not have their medical checkups within six months. In patients who did, reduced cardiac muscle function persisted in over a third of them. Within this group, only a quarter of those who met the criteria of getting an implanted defibrillator were referred to a specialist to get one installed.
One in three heart attack survivors in Canada fail to adhere to the recommended medical guideline of getting a medical check-up three to six months after their attack.
Heart attacks often weaken the cardiac muscle and reduce its ability to pump blood. Weak cardiac muscles increase heart attack survivors’ risk of sudden cardiac death (SCD).
Rechecking the heart’s pumping function, usually with an ultrasound or ‘echo’, helps monitor the condition of cardiac muscles. In cases where they have weakened further, doctors will often recommend additional drug therapy or implanted defibrillators.
A CANet study tracking over 500 heart-attack survivors across Canada found that one in three patients with reduced cardiac muscle function after a heart attack did not have their medical checkups within six months (results published in JAMA Network Open). In patients who did, reduced cardiac muscle function persisted in over a third of them. Within this group, only a quarter of those who met the criteria of getting an implanted defibrillator was referred to a specialist to get one installed.
“We wanted to find out how many patients get a medical check-up at the recommended time and whether they end up receiving the recommended treatments,” says CANet investigator Stephen B. Wilton, who led the study.
The investigation found that the most common reason for not having a medical check-up was that it was not physician-ordered.
▼ show more
Wilton recommends doctors to adhere to the three-month follow-up guideline because, “it is difficult to know without testing if cardiac muscle function has improved, worsened, or stayed the same in someone who has survived a heart attack.”
Currently, the team is implementing a module through CANet’s VIRTUES platform that encourages heart-attack survivors to get follow-up medical check-ups, and suggests ways to lead a healthy lifestyle.
“Self-empowerment is key,” Wilton says. “If you are a heart-attack survivor, educate yourself on the medical consequences. Inquire about follow-up medical check-ups, while, of course, taking medication, going to cardiac rehabilitation, and leading a healthy lifestyle.”
▲ show less
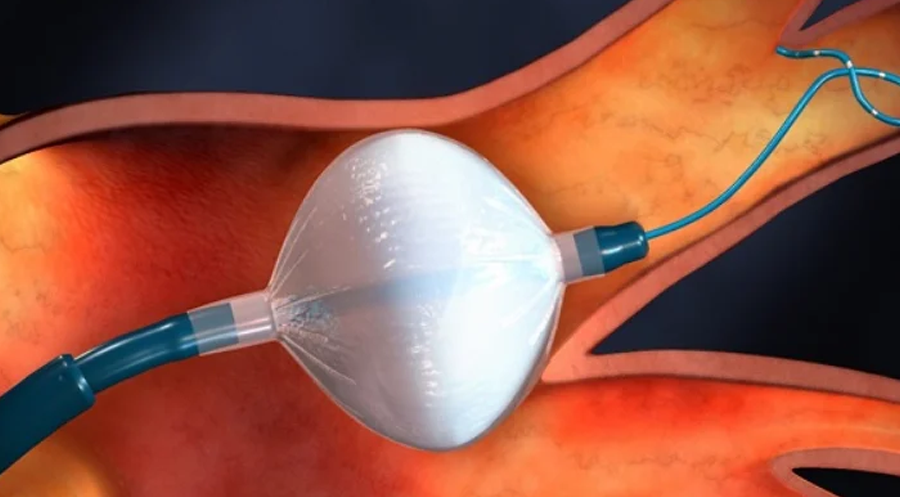
Medtronic Arctic Front cryoballoon
CANet-funded project fulfils a critical need for minimally invasive cardiac procedures that improve patient outcomes without increasing healthcare costs and treatment time to reduce the burden of atrial fibriallation in Canada.
A CANet project aimed at reducing atrial fibrillation (AF) hospitalizations in Canada using a revolutionary new treatment has successfully concluded its first clinical trial (results published in the New England Journal of Medicine).
AF, a heart rhythm disorder caused by faulty heart tissues, results in rapid, irregular heartbeats. Patients are at a greater risk for stroke and death.
CANet investigator Dr. Jason Andrade pioneered an AF treatment that freezes faulty heart tissues while minimizing damage to surrounding areas.
Dr. Andrade teamed up with CANet industry partners Medtronic and Baylis Medical to evaluate the new technology – cryoablation – that lowers the risk for arrhythmia recurrence and stroke, and prevents the progression of AF.
“This is a major advancement in the interventional treatment of AF and a significant Canadian accomplishment,” Dr. Andrade says.
Significantly, it reduces the patient’s dependence on antiarrhythmic drugs (AADs), which are ineffective and have severe side effects such as heart failure or organ toxicity.
▼ show more
Over 300 patients across Canada participated, making it the most extensive randomized study to date in this patient population. Patients were intensely monitored for up to a year after treatment. The trial showed that cryoablation as the initial treatment improves both life quality of life and symptoms compared with medical therapy.
Dr. Andrade’s CANet-funded project fulfills a critical need for minimally invasive cardiac procedures that improve patient outcomes without increasing healthcare costs and treatment time to reduce the burden of AF in Canada. A significant portion of AF-related healthcare costs comes from hospitalization and acute care.
▲ show less

Sheldon Cheskes, CANet Investigator with an AED Drone
In a recently concluded test conducted in rural Ontario, Drone Delivery Canada found that drones delivered Automated External Defibrillators (AEDs) more quickly compared to paramedics. The drones were flown remotely from a control centre almost 40 kilometres away.
CANet plays a crucial role in saving cardiac arrest patients in rural communities across Canada by helping develop drones that quickly deliver life-saving devices to bystanders.
The first few minutes after a cardiac arrest are critical.
Cardiac arrest survival rates are worse in rural communities compared to urban areas. Ambulance and fire services have slower response times. The public often does not know how to operate Automated External Defibrillators (AEDs) – devices used to ‘shock’ the heart to restore its normal rhythm.
Sheldon Cheskes’ CANet-funded project, “AED On The Fly,” is pioneering how Canada deals with cardiac arrest. It is the first project of its kind to research the potential implementation of AED-equipped drones as part of an EMS response.
The future of cardiac arrest response in rural communities would significantly change. Our vision is that when a 911 call comes in for a cardiac arrest victim, a drone equipped with an AED is dispatched, along with ambulance and fire crews. Bystanders follow the instructions provided by a dispatcher to simplify the use of the AED and save lives.
“Drones have the potential to arrive earlier than firefighters and ambulances to the scene of a cardiac arrest in these communities, and those extra minutes could be life-savers,” says Cheskes, a CANet Investigator, medical director at Sunnybrook Centre for Prehospital Medicine, and professor of medicine at the University of Toronto.
▼ show more
CANet’s Commercialization Grant helped Cheskes work with Drone Delivery Canada (DDC) and Indro Robotics to develop and refine the technology to reduce response times and potentially save lives.
In simulation testing conducted in the Town of Caledon and the Renfrew County, Ontario, Cheskes found that drones delivered AEDs more quickly than paramedics during a mock 911 response with flight distances of 7-10 kilometres. During one set of flights, the drones were flown remotely from a control centre almost 40 kilometres away.
The CANet-funded project could potentially expand to other emergencies such as delivering epinephrine for anaphylactic shock, naloxone for opioid overdose and medical kits for trauma victims.
▲ show less
A CANet project is creating Canada’s first set of guidelines for emergency room (ER) physicians that standardize acute atrial fibrillation and flutter (AAFF) treatment across the country, reducing the length of patients’ stay by 21%.
The project has successfully implemented its AAF Best Practices Guidelines into 11 large emergency rooms in five provinces, with plans to be adopted over 1000 sites across Canada.
Most ERs in Canada treat AAFF – abnormally rapid heart rates that have been present for less than seven days and are often disabling to most patients – by using drugs or electricity to help return the heart to its normal ‘sinus’ rhythm. The procedure is known as cardioversion. Patients are usually discharged soon after that.
CANet Investigator Ian Stiell is an ER physician at The Ottawa Hospital Research Institute. His ER group has maintained a low admission rate of less than five per cent for many years with an excellent safety record.
Stiell created the treatment guidelines by combining his ER experience and conversations with patients, ER physicians, and cardiologists from rural, community, and academic centres.
“We have seen more and more Canadian ER physicians willing to cardiovert AAFF patients and then discharge them directly home from the ER,” Stiell says. “We want to encourage ER physicians working in small, medium, and large hospitals across Canada to adopt the guidelines.”
▼ show more
By funding his work to help decrease ER admissions for AAFF cases, CANet is helping Stiell take the success story Canada-wide.
His CANet-funded project is currently on a two-year trial to evaluate the effectiveness of the guidelines in 11 Canadian ERs across Nova Scotia, New Brunswick, Quebec, and Ontario.
The hope is to ease the pressure from an already over-burdened Canadian healthcare system and reduce ER visits by 30 percent.
Already endorsed by the Canadian Association of Emergency Physicians, the hope is the guidelines will ease the pressure from an already over-burdened Canadian healthcare system and reduce ER visits by 30 percent.
▲ show less

Venkatesh Thiruganasambandamoorthy, CANet Investigator
The Canadian Syncope Risk Score (CSRS) is able to help emergency room physicians determine if a patient is at risk for ventricular arrhythmia and whether they should be admitted. Very-low-risk and low-risk patients could generally be discharged, while brief hospitalization could be considered for high-risk patients.
Hospital News
Projected to save the Canadian healthcare system approximately $70M per year, the CANet-funded Canadian Syncope Risk Score (CSRS) is helping doctors improve syncope care in the emergency room (ER), reducing the burden on hospitals throughout Canada.
Syncope is the temporary loss of consciousness due to the incomplete delivery of oxygen to the brain. A complete recovery immediately follows it. In some high-risk cases, syncope eventually leads to potentially fatal conditions like arrhythmias.
Syncope accounts for one to three percent of all emergency department visits.
Before creating the CSRS tool, doctors did not have standardized guidelines on evaluating syncope patients, differentiating between low- and high-risk cases, which patients to send back home, and whom to assess further.
The CSRS tool will result in 71% of all syncope patients being discharged quickly from the ER (within 2 hours).
Developed by CANet Investigator, the University of Ottawa Epidemiology and Community Medicine professor, Ottawa Hospital Research Institute scientist, and Ottawa Hospital doctor Venkatesh Thiruganasambandamoorthy, the CSRS helps physicians better identify which ER syncope patients need to be admitted, and which ones can be safely followed up in an outpatient clinic.
CSRS was successfully validated in a recent trial held in nine emergency departments across Canada.
▼ show more
It found that the Score helped ER physicians accurately predict 30-day serious outcomes for syncope patients after being released from the ER. They could determine if a patient was at risk for ventricular arrhythmia and whether they should be admitted. Very-low-risk and low-risk patients could generally be discharged, while brief hospitalization could be considered for high-risk patients.
“We believe CSRS implementation has the potential to improve patient safety and health care efficiency,” Thiruganasambandamoorthy says.
▲ show less
The comprehensive and unique Canadian Sudden Cardiac Arrest Network Registry will help understand the causes and outcomes of sudden cardiac arrest, which affects almost 45,000 Canadians each year, many of who die from it.
Canada’s first comprehensive database of sudden cardiac arrest (SCA) cases is being developed with the help of CANet.
Co-led by CANet investigators Dr. Paul Dorian, a University of Toronto Medicine professor, and Dr. Steve Lin, a University of Toronto Emergency Medicine Assistant Professor, the Canadian Sudden Cardiac Arrest Network Registry (C-SCAN) is a comprehensive, unique registry that will help understand SCA causes and outcomes.
SCA affects close to 35,000 Canadians each year, of which close to 90% die.
“The C-SCAN project, with its detailed tally of SCA cases, patient histories, and other details – location of the SCAs, actions taken by paramedics, patient survival rates, for example – will be critical for predicting, preventing, and reducing SCA cases,” Dorian says. It will also help improve the lives of those who survive it.
The CANet-funded project successfully advocated for a mandatory AED registry in Ontario. It helped draft legislation to create a compulsory Provincial AED registry, Bill 141 Defibrillator Registration and Public Access Act, 2020. This legislation received royal assent in June 2020.
C-SCAN combines information from three sources – the Canadian Resuscitation Outcomes Consortium‘s (CanROC) database of SCA cases, in-hospital data from the Canadian Institutes of Health Information, and uniquely, coroner’s reports – a vital trove of health-related information, usually buried under slow-moving administrative and bureaucratic procedures.
▼ show more
Dorian highlights several potential outcomes of the CANet-funded C-SCAN project – educating the public to recognize warning signs of an impending SCA, teaching them to use Automated External Defibrillators (AEDs), and strategically placing AEDs in easy-to-find locations throughout buildings, and public spaces.
Apart from the registry itself, C-SCAN also consists of a national network of scientists, emergency physicians, cardiologists, coroners, medical examiners, and patients from across Canada.
▲ show less